Causes of Asthma and Best Practices for Prevention
Working with your physician to ensure long-term control can help you prevent the development of life-threatening causes of asthma. A combination of genetic and environmental factors are likely to cause asthma
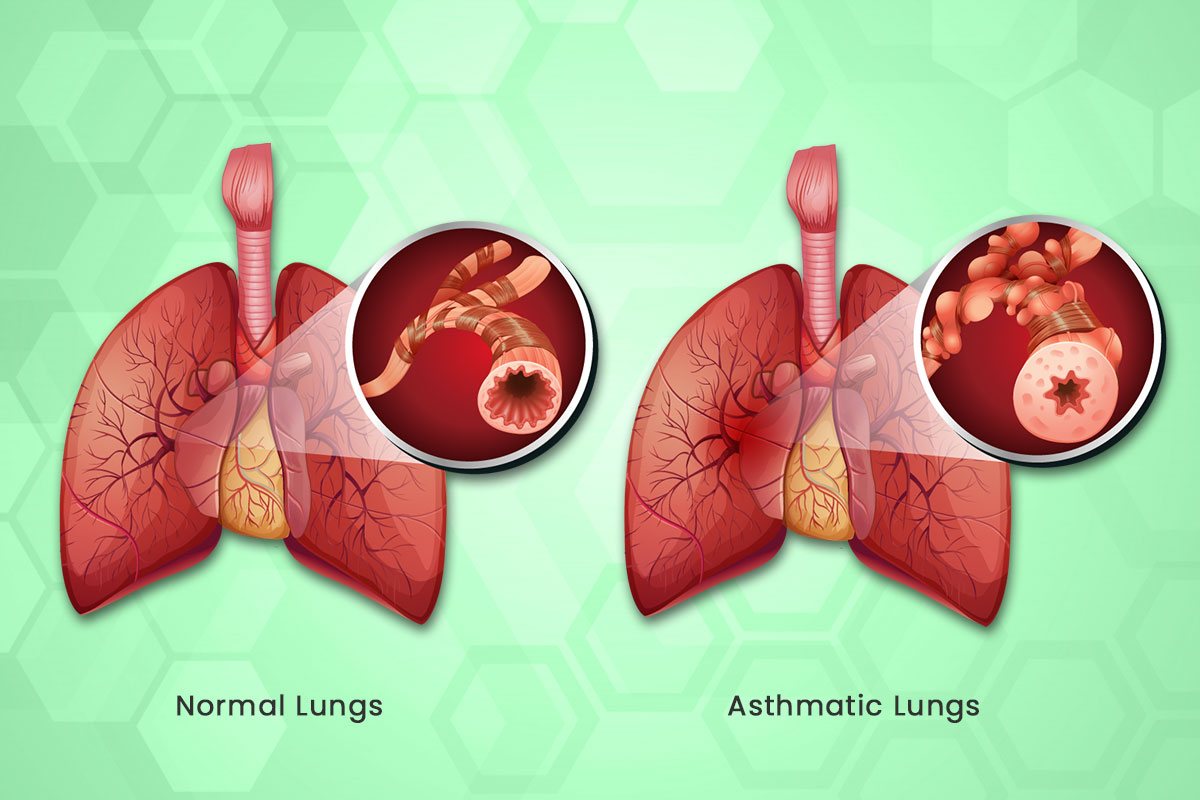
Asthma is a disease that affects your lungs. It causes your airways to narrow and swell and may produce extra mucus obstructing the outflow of air from the lungs. This can make breathing difficult leading to shortness of breath, triggering coughing and wheezing when you breathe out. Causes of Asthma widely vary from family history to allergies and obesity.
Asthma is one of the most common chronic condition. It affects both adults and children almost equally (slightly higher in children 5-14 years). It has a higher preponderance in female gender. Preponderance ethnically is highest amongst blacks, followed by Hispanics then whites. In the US about 25 million people (8% US population) had asthma in 2017 (data from CDC).
For some people, asthma can be a minor nuisance. For others, however, it can be a major problem interfering with daily activities and potentially leading to a life-threatening asthma attack.
Also Read: Lung Cancer Awareness – Symptoms, Stages and Treatment
Unfortunately, asthma cannot be cured completely. The good news is symptoms can be controlled. Asthma in relation to the environment and your body can change over time. Severe asthma may not remain severe or mild asthma could become worse and more frequent. Additionally, there are many triggers that could cause an asthma attack. Therefore, it is important to work with your doctor and adjust treatment as needed.
Signup today and find a doctor near you
Causes of Asthma/Risk factors
It is not entirely clear what causes asthma. It is likely due to a combination of genetic and environmental factors.
There are several triggers which can exacerbate underlying asthma which we will discuss later. There are several risk factors that are thought to increase your chances of developing asthma.
- Family history – Having a parent or sibling with asthma can make you upto six times more likely to develop asthma.
- Occupational exposure – Exposure to certain elements or fumes at work can cause asthma to develop for the first time.
- Respiratory infections – Some children who experience viral respiratory tract infections in infancy or childhood can go on to develop asthma.
- Allergies – Having an allergic condition such as eczema (atopic dermatitis) or hay fever (allergic rhinitis) can be a risk factor for developing asthma.
- Smoking – Cigarette smoking causes irritation to the airways; secondhand smoke can also be detrimental. Additionally, children whose mothers smoked during pregnancy may also be more likely to develop asthma.
- Obesity – One of the leading causes of Asthma affecting both children and adults.
Symptoms
Symptoms vary greatly from person to person. Some people have mild symptoms and only seldom. Others have more frequent, debilitating disease. Symptoms most commonly include shortness of breath, wheezing, cough, and chest tightness.
Signs that your asthma is worsening include increased frequency of asthma attacks, increased need to use an inhaler, or worsened readings with a device used to measure your breaths – a peak flow meter.

Prevention
You can, with the help of your doctor, design a step-by-step plan to help reduce the occurrence of asthma attacks. The following are some tips.
- You can identify and avoid asthma triggers. There are numerous possible triggers for asthma. Airborne allergens, such as pollen, pet dander, dust mites, mold spores, etc. may cause asthma attacks. Respiratory infections, cold air (worse with exercise), air pollutants such as fire ash, smoke or occupational from environmental particles/allergens may be culprits. Certain medical conditions, such as GERD (gastroesophageal reflux disease) can cause reflux of stomach acids into your throat. Lastly, certain medications including β-blockers (mainly nonselective β-blockers like Propranolol), Aspirin, NSAIDs (Ibuprofen, Aleve) can cause an asthma exacerbation.
- Identify and treat attacks early. Working with your physician to ensure good long-term control can help you have less frequent asthma symptoms. And in turn prevent the possibly life-threatening causes of asthma.
- Take your medications on time and as prescribed. Ensuring that you are taking your medications regularly is crucial to establishing control over your asthma symptoms.
- Be cognizant of how often you are needing to use your rescue inhaler. This can be a warning sign of worsening underlying disease or a pending severe asthma attack. For example, feeling the need to use your inhaler more frequently than normal is a red flag and should cause you enough concern to seek medical advice.
- Get immunized against COVID-19, influenza and pneumonia.
Also Read: Chest Pain – Causes, Effects, Diagnosis and Treatment
Diagnosis
For the diagnosis of asthma, you may need to undergo a history and physical exam with your doctor, and a lung function test.
A lung function test will help determine how well you exhale air from your lungs. Lung function tests are done before and after inhaling a medication known as a bronchodilator. Bronchodilators relax your airways and allow them to dilate or open. If you have significant improvement on your lung function test with the use of a bronchodilator, you most likely have asthma.
Treatment
In addition to lifestyle modification, there are several types of medications available to treat asthma. Each person’s asthma is different and requires a treatment plan crafted to your needs by your physician. For example, if obesity is identified as a cause of asthma and a risk factor, weight loss can help. Some asthma medications work more quickly to relax your airways and help you breathe easier immediately. While other, longer acting treatments reduce the swelling and inflammation in your airways and prevent symptoms.







